Why I Avoid Sinus Surgery: Effective Sinus Surgery Alternatives For Chronic Sinusitis

The patient sitting across from me was desperate. Three sinus surgeries, countless medications, and still suffering from chronic sinusitis. “Doctor,” she said, with tears in her eyes, “what would you do if this were your own family?”
Every week in my Huntsville ENT clinic, I meet people who have been told surgery is their only option. Some have never tried a focused, step by step plan. Others already went through surgery and got only short relief. A few feel worse than before and now worry they made a mistake.
After years as an ENT surgeon, I’ve learned something that surprises many patients. Most sinus surgeries can be avoided when you take a conservative sinus treatment approach seriously. You still need good testing. You still need a clear diagnosis. But you do not need to rush to the operating room in most cases.
Here, I’ll walk you through the sinus surgery alternatives I use, why I often choose non-surgical sinus therapy first, when surgery truly helps, and what you should ask before you agree to any procedure.
The hard truth about sinus surgery success rates
Surgery is often helpful, but it is not a Every week in my Huntsville ENT clinic, I meet people who have been told surgery is their only option. Some have never tried a focused, step by step plan. Others already went through surgery and got only short relief. A few feel worse than before and now worry they made a mistake.
Endoscopic sinus surgery, including functional endoscopic sinus surgery (FESS), can:
- open the sinuses to improve ventilation and drainage
- remove polyps
- improve access for topical treatments after surgery
Those goals are clearly stated in standard definitions of FESS.
But here is what many people do not hear early enough: surgery usually starts a long relationship with ongoing medical care. You should expect to continue sinus medications after surgery, even when surgery goes well. Some patients need less medication later, but ongoing care is still common.
So if you feel pressured with a promise like “this will fix you,” pause. That is not how chronic sinus disease usually behaves.
Revision surgery is real
One reason I tend to avoid sinus surgery when it is not clearly needed is simple. Some patients end up needing more surgery.
A large database study of over 61,000 patients found that 6.65% returned for revision endoscopic sinus surgery during the study period, and the risk increased in patients with nasal polyps and in women. In that same analysis, revision rates at 5 years were estimated around 7.9% for chronic rhinosinusitis without polyps and 9.9% for chronic rhinosinusitis with polyps.
Long-term prospective data also shows revisions add up over time. In a study with about 11 years of follow-up, the revision surgery rate reached 17% overall, and 25% in chronic rhinosinusitis with polyposis.
Many patients improve after surgery and stay improved. Still, it means repeat procedures are part of the reality for a meaningful group of people.
When a patient has already had one surgery, the next decision becomes harder. Scar tissue, healing patterns, and ongoing inflammation can make each step more complex.
Sinus surgery complications are uncommon, but they matter
Even when complication rates are low, the stakes can be high.
A large TriNetX analysis covering 2005 to 2024 reported specific post-operative complication rates after endoscopic sinus surgery. It found:
The same analysis reported 1.47% 30-day readmission and 1.62% emergency department visits within 30 days.
Some major medical centers also list risks like:
- bleeding
- recurrence of disease
- spinal fluid leak with risk of meningitis
- visual problems, including very rare but serious vision loss
My conservative sinus surgery alternative protocol
When someone comes in asking about sinus surgery alternatives, I start by clarifying what problem we are actually treating.
Step 1: Confirm what type of sinus problem you have
Not every stuffy nose is chronic sinusitis. Not every facial pressure is a sinus infection. The first job is correct diagnosis.
A major adult sinusitis guideline stresses the need to distinguish acute bacterial rhinosinusitis from viral causes and other noninfectious conditions. It also says chronic rhinosinusitis should be confirmed with objective evidence of inflammation using anterior rhinoscopy, nasal endoscopy, or computed tomography.
If you have symptoms that fit chronic rhinosinusitis, the definition includes at least 12 weeks of symptoms, with at least two symptoms and objective evidence on endoscopy or CT. That is a key point. Chronic symptoms alone do not finish the diagnosis.
This is one reason I often avoid rushing to surgery. If the diagnosis is shaky, the surgery decision will be shaky too.
Look for factors that change the plan
The same guideline highlights that some chronic conditions can modify how rhinosinusitis should be managed, including:
- asthma
- cystic fibrosis
- immunocompromised state
- ciliary dyskinesia
So I ask targeted questions and review the bigger picture. If you treat only the nose and ignore the rest, you often get poor results.
Use proven medical therapy tools, in the right order
The adult sinusitis guideline recommends saline nasal irrigation, topical intranasal corticosteroids, or both for symptom relief of chronic rhinosinusitis.
It also lays out options for acute bacterial rhinosinusitis. Clinicians may offer watchful waiting without antibiotics or prescribe initial antibiotic therapy for uncomplicated cases. If an antibiotic is chosen, the guideline recommends amoxicillin with or without clavulanate for 5 to 10 days as first-line therapy. It also stresses reassessment if the patient fails to improve by 7 days or worsens.
For chronic bacterial sinusitis, clinical indicators describe oral antibiotics of 2 to 4 weeks duration, culture-directed when appropriate, along with systemic and or topical steroids at the clinician’s discretion, plus saline irrigations as an option. They also list treatment of allergic rhinitis with avoidance measures, pharmacotherapy, and or immunotherapy at the clinician’s discretion.
Step 4: Upgrade your irrigation technique
Many people say, “I tried saline.” Then I ask what they used, how often, what volume, what device, and what their technique looked like.
A Cochrane review found that low-volume nebulized saline did not outperform intranasal steroids. But daily large-volume (150 ml) hypertonic saline irrigation showed some benefit compared with placebo, though the evidence quality was low and very low at different time points. The same review reported side effects in the saline group, including nosebleeds, with 23% reporting side effects in that trial.
Another multicenter survey study found high-volume devices were most effective for clearing secretion in several rhinosinusitis groups and helped reduce post-nasal drip in acute bacterial rhinosinusitis. It also documented adverse events such as retained fluid in the sinuses, salty taste, and ear pain or hearing loss.
If you develop nose bleeds or your ears hurt, we adjust.
I also remind patients that saline can feel strange at first. Many people need coaching and practice. That is normal.
Step 5: Consider steroid irrigation carefully, with clear counseling
Many patients ask about adding steroids to rinses.
A systematic review covering 2012 to 2024 reported that high-volume steroid nasal irrigations showed superior efficacy compared to sprays in several studies, particularly after surgery, and did not show significant adrenal suppression or increases in intraocular pressure in the reviewed safety evaluations. Minor adverse events did occur.
So what do I do with that?
I treat steroid irrigation as a tool that may help in selected situations and often recommend them.
Step 6: Address suspected biofilm and microbial issues without “antibiotics forever”
Chronic rhinosinusitis is not always a simple bacterial infection.
A narrative review of non-antibiotic antimicrobial agents discussed how dysbiotic flora and biofilm colonization may be therapeutic targets. It reviewed topical therapies such as:
- Xylitol
- manuka honey
- baby shampoo irrigation
- colloidal silver
- Povidone-iodine
- Bacteriophages
- Lactoferrin
- carrageenan
But they emphasized that many studies have low evidence levels and limited safety data.
This is where patients often ask, “What else can I do?”
That same review highlighted xylitol as having the best level of evidence among the agents discussed, with multiple studies suggesting symptom improvement compared with saline, though more research is still needed. It also described mixed or inconclusive results for several other agents, and noted that nasal irritation and stopping therapy can happen with baby shampoo irrigation.
I handle these options in a structured way. I pick a plan that matches your condition, your tolerance, and the level of evidence we have.
Step 7: Reassess, do not drift
Conservative care only works when you reassess the response and confirm the diagnosis. If you worsen, if you do not improve, or if red flags appear, then the plan must change. The adult sinusitis guideline specifically calls for reassessment when symptoms fail to improve with initial management.
This is one reason my patients like the conservative approach. It feels active. It has checkpoints.
When I actually recommend sinus surgery
Even though I often avoid sinus surgery, I do recommend it sometimes. The key is that surgery should have a clear target and a clear reason.
Exception 1: Structural or disease patterns that medicine cannot fix
There are cases where anatomy or disease type makes medical therapy unlikely to succeed on its own.
Clinical indicators for adult endoscopic sinus surgery list several histories where surgery is considered, including chronic rhinosinusitis with persistent symptoms plus objective evidence that is refractory to optimal medical treatment, allergic fungal rhinosinusitis, unilateral paranasal sinus opacification that suggests specific disease processes, complications of sinusitis with extension to nearby structures, mucocele, and recurrent acute rhinosinusitis.
Exception 2: Nasal polyps that create obstruction or repeated relapse
Polyps matter. Multiple guidelines and studies point to this subgroup as different.
The adult sinusitis guideline recommends confirming the presence or absence of nasal polyps in chronic rhinosinusitis. Clinical indicators include chronic rhinosinusitis with nasal polyps that is refractory to medical treatment, and sinonasal polyposis with nasal airway obstruction or suboptimal asthma control as scenarios where surgery may be appropriate.
Research also shows polyps connect to revision risk. In the large revision database study, nasal polyps predicted higher likelihood of revision surgery. In the long-term outcomes study, revision rates were higher in the polyposis group.
So why recommend surgery at all in polyps?
Because in the right patient, surgery can reduce obstruction and improve access for topical therapy afterward. Also, modern medical options have expanded. For severe chronic rhinosinusitis with nasal polyps, a biologic like dupilumab improved polyp size, congestion, and CT scores compared with placebo in phase 3 trials.
In other words, polyps can justify surgery in some cases, but polyps also justify serious non-surgical therapy. The plan should match the severity and goals.
Exception 3: Failed conservative therapy with a clear surgical target on imaging and endoscopy
This is the most common situation where surgery becomes reasonable. You tried appropriate therapy, you still suffer, and the workup points to a target that surgery can address.
Clinical indicators note imaging is generally obtained after optimal medical therapy, unless early imaging is needed due to concern for complications or alternative diagnosis. They also highlight CT as the preferred imaging study for surgical planning.
A prospective study explored the role of Lund-Mackay CT score in predicting prognosis of FESS and suggested that patients with higher scores in their sample had statistically significant symptom improvement, while lower scores did not show the same outcome pattern.
CT score supports what many surgeons see. A stronger objective disease burden may align with clearer surgical benefit in some patients.
I also follow principles from surgical management guidance that emphasize confirming diagnosis, assessing candidacy based on symptoms, disease characteristics, quality of life, and prior therapy. I also take seriously the idea that you do not force a one-size-fits-all medical regimen length before surgery.
When surgery is truly needed, my counseling changes. I speak plainly about expectations, the chance of chronicity or relapse, and the likelihood of long-term medical management afterward, tailored to disease subtype. I also go over postoperative care needs like follow-up, debridement when clinically warranted, and warning signs such as excessive bleeding, vision changes, severe headache, mental status changes, and possible CSF leak concerns.
What patients really need to know about sinus surgery alternatives
If you are trying to avoid sinus surgery, you need two things. You need a real plan, and you need the right questions.
Questions to ask your ENT before you agree to surgery
Here are questions I believe every patient should ask:
- What is my exact diagnosis? Do I meet criteria for chronic rhinosinusitis, recurrent acute rhinosinusitis, or something else?
- What objective evidence confirms inflammation? Did you see it on nasal endoscopy, anterior rhinoscopy, or CT?
- Do I have nasal polyps? If yes, how does that change the plan?
- What medical therapies have I tried, and were they done correctly? This includes saline irrigation technique and topical intranasal corticosteroids.
- Is watchful waiting reasonable if you think this is acute bacterial rhinosinusitis? The adult guideline supports watchful waiting or antibiotics in uncomplicated cases.
- If antibiotics are needed, what is the plan for reassessment? The same guideline calls for reassessment if you do not improve or you worsen.
- Are you considering testing for allergy and immune function? That is listed as an option in chronic rhinosinusitis evaluation.
- What conditions might be modifying my sinus disease? Asthma and other chronic conditions can change management.
- What are the specific risks for me? Ask about bleeding, orbital complications, CSF leak, meningitis, and emergency visits. Those risks show up in complication analyses.
- If surgery helps, what is the goal of surgery in my case? Better drainage, removing polyps, improving access for topical therapy, cultures, tissue diagnosis, or all of these?
- What follow-up will you do after surgery, and when? Routine follow-up with symptom review and nasal endoscopy in the months after surgery is part of modern guidance.
Red flags that suggest you are being rushed
You should be cautious if:
- You are told you have chronic rhinosinusitis with no objective confirmation.
- You are offered surgery without nasal endoscopy or CT in a non-urgent case.
- Your clinician dismisses saline irrigation and topical steroids as “optional extras,” even though they are recommended for symptom relief in chronic rhinosinusitis.
- No one asks about modifying conditions, such as asthma or immune problems, which can change the treatment plan.
- The discussion ignores long-term management after surgery and talks as if surgery ends the problem.
Realistic timelines for improvement with non-surgical therapy
People want quick relief. I understand that.
But chronic rhinosinusitis is, by definition, chronic. It often takes sustained care.
In the saline irrigation evidence, benefits in one trial became more noticeable over months, with more effect seen at six months than at three months in that study. That fits what I see clinically. It can take time for inflammation to calm down and for habits and technique to settle in.
I usually frame it this way: expect a significant improvement within 4 weeks of optimal medical treatment, with the possibility of continued improvement over the next several months.
Final words
Surgery has a place. It can help selected patients a great deal. Yet it is not a cure alone and in itself, revision surgery is a real possibility, and sinus surgery complications, while uncommon, can be serious.
For most people, the best path starts with sinus surgery alternatives. Confirm the diagnosis with objective evidence. Identify polyps and other modifying conditions. Use conservative sinus treatment that includes saline irrigation and topical intranasal corticosteroids, as recommended in major guidance. Reassess carefully. Upgrade technique, not just prescriptions. Consider emerging non-surgical sinus therapy options when appropriate.
If you are considering sinus surgery or someone told you it is your only option, I encourage you to slow down and ask better questions. A thoughtful plan can change everything.
If you want help sorting out your specific situation, schedule a consultation so we can review your symptoms, your exam, and your imaging and map out the most conservative plan that still gives you the best chance at real relief.
Frequently Asked Questions
Do most people with chronic sinusitis need surgery?
No. Most people do not need surgery right away. You should first confirm the diagnosis and try focused medical care, like saline rinses and nasal steroid sprays.
What should I try before sinus surgery?
You should try large-volume saline irrigation, intranasal corticosteroid sprays, and treatment for allergies if present. In some cases, you may need culture-directed antibiotics.
How do I know if I truly have chronic rhinosinusitis?
You need at least 12 weeks of symptoms plus objective proof of inflammation on nasal endoscopy or CT scan. Symptoms alone are not enough.
Can saline rinses really make a difference?
Yes, when done correctly. High-volume rinses used daily often work better than quick sprays. Technique and consistency matter.
What if I have nasal polyps?
Polyps can change the plan. Some patients improve with medical therapy. Others may need surgery if polyps cause blockage or keep coming back.
Is sinus surgery a cure?
Not alone and by itself. Surgery can improve drainage and remove blockages, but most people still need ongoing medical care afterward.
What are the risks of sinus surgery?
Serious problems are uncommon but can include bleeding, eye injury, spinal fluid leak, or infection. Even small risks matter when it’s your health.
When is surgery clearly necessary?
Surgery may be needed if you fail proper medical therapy, have severe polyps, or develop complications that affect the eyes or brain.
How long should I try conservative treatment?
You should reassess within 4 weeks. Chronic sinus disease usually improves step by step, not overnight.
What questions should I ask before agreeing to surgery?
Ask about your exact diagnosis, proof of inflammation, whether you have polyps, what treatments you’ve tried, and what the real goal of surgery is in your case.
Sources
- Stein, N. R., Jafari, A., & DeConde, A. S. (2017). Revision rates and time to revision following endoscopic sinus surgery: A large database analysis. Laryngoscope, 128(1), 31–36.
- Smith, T. L., Schlosser, R. J., Mace, J. C., Alt, J. A., Beswick, D. M., DeConde, A. S., Detwiller, K. Y., Mattos, J. L., & Soler, Z. M. (2019). Long-term outcomes of endoscopic sinus surgery in the management of adult chronic rhinosinusitis. International Forum of Allergy & Rhinology, 9(8), 831–841.
- Fischer, J. L., Gallagher, T. J., Lin, M. E., Kim, I., Wrobel, B. B., Beswick, D. M., Lee, J. T., Wang, M. B., & Suh, J. D. (2025). Complications in endoscopic sinus surgery: A TriNetX network analysis. International Forum of Allergy & Rhinology, 15(12), 1393–1404.
- Rosenfeld, R. M., Piccirillo, J. F., Chandrasekhar, S. S., Brook, I., Kumar, K. A., Kramper, M., Orlandi, R. R., Palmer, J. N., Patel, Z. M., Peters, A., Walsh, S. A., & Corrigan, M. D. (2015). Clinical practice guideline (update): Adult sinusitis. Otolaryngology–Head and Neck Surgery, 152(2 Suppl), S1–S39.
- Chong, L. Y., Head, K., Hopkins, C., Philpott, C., Glew, S., Scadding, G., Burton, M. J., & Schilder, A. G. M. (2016). Saline irrigation for chronic rhinosinusitis. Cochrane Database of Systematic Reviews, 2016(4), Article CD011995.
- Piromchai, P., Puvatanond, C., Kirtsreesakul, V., Chaiyasate, S., & Suwanwech, T. (2020). A multicenter survey on the effectiveness of nasal irrigation devices in rhinosinusitis patients. Laryngoscope Investigative Otolaryngology, 5(6), 1114–1120.
- Bernstein, J. A., White, A. A., Han, J. K., Lang, D. M., Elkayam, D., & Baroody, F. M. (2023). Review of evidence supporting the use of nasal corticosteroid irrigation for chronic rhinosinusitis. Annals of Allergy, Asthma & Immunology, 130(1), 46–57.
- Caetano, J. V. B., Valera, F. C. P., Anselmo-Lima, W. T., & Tamashiro, E. (2024). Non-antibiotic antimicrobial agents for chronic rhinosinusitis: A narrative review. Brazilian Journal of Otorhinolaryngology, 90(4), Article 101436.
- Bachert, C., Han, J. K., Desrosiers, M., Hellings, P. W., Amin, N., Lee, S. E., Mullol, J., Greos, L. S., Bosso, J. V., Laidlaw, T. M., Cervin, A. U., Maspero, J. F., Hopkins, C., Olze, H., Canonica, G. W., Paggiaro, P., Cho, S. H., Fokkens, W. J., Fujieda, S., … Mannent, L. P. (2019). Efficacy and safety of dupilumab in patients with severe chronic rhinosinusitis with nasal polyps (LIBERTY NP SINUS-24 and LIBERTY NP SINUS-52): Results from two multicentre, randomised, double-blind, placebo-controlled, parallel-group phase 3 trials. The Lancet, 394(10209), 1638–1650.
- Singh, G. B., Arora, N., Tomar, S., Kwatra, D., & Kumar, S. (2020). The role of sinus CT in surgical treatment decisions for chronic rhinosinusitis. American Journal of Otolaryngology, 41(6), Article 102729.
- Chapurin, N., Khan, S., & Soler, Z. M. (2023). Economics of medical and surgical management of chronic rhinosinusitis with nasal polyps: A contemporary review. American Journal of Rhinology & Allergy, 37(2), 123–131.
- Scangas, G. A., Su, B. M., Remenschneider, A. K., Shrime, M. G., & Metson, R. (2016). Cost utility analysis of endoscopic sinus surgery for chronic rhinosinusitis. International Forum of Allergy & Rhinology, 6(6), 582–589.
Related Posts
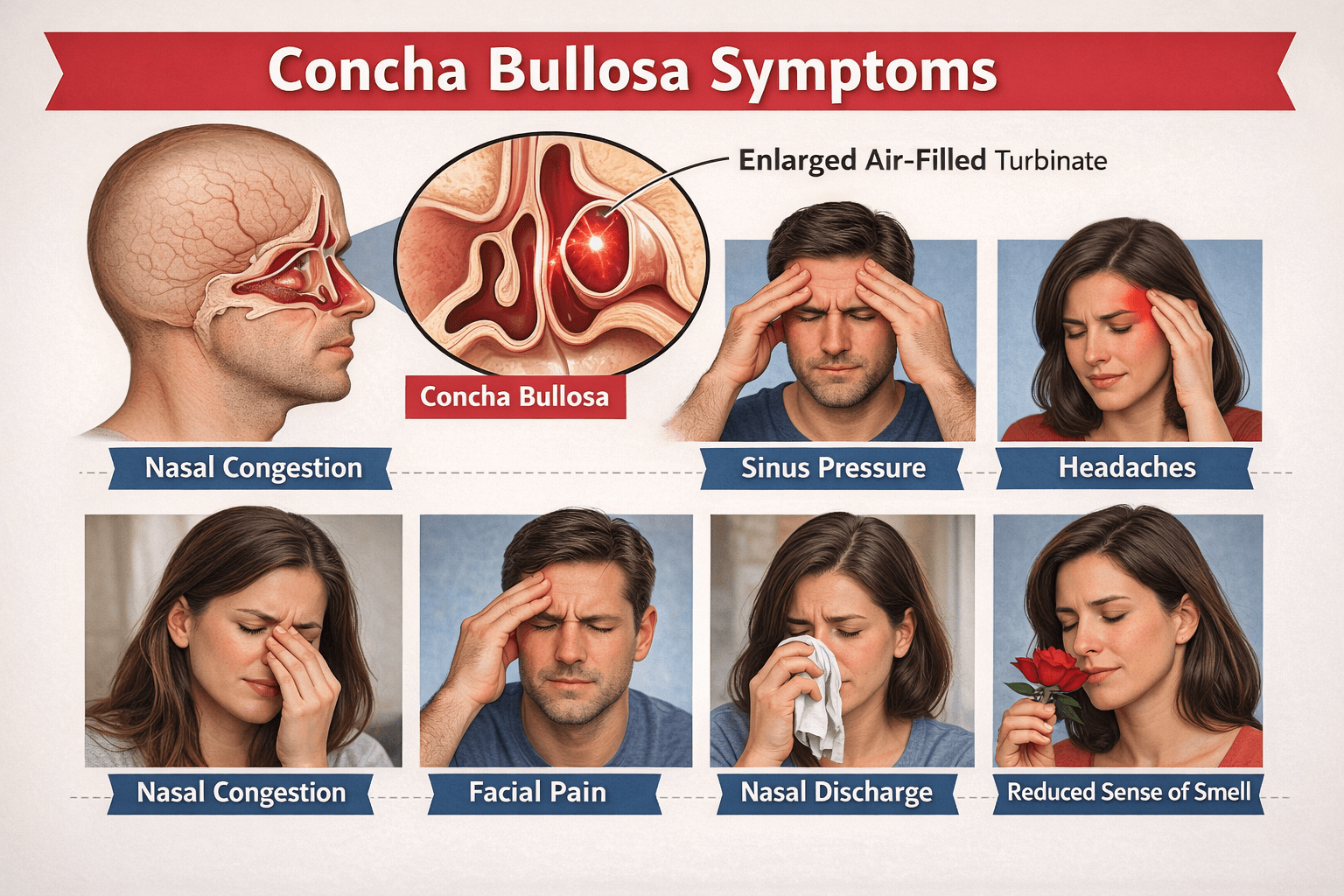
Concha Bullosa symptoms and treatment: How I explain it to my patients