How the Posterior Nasal Nerve Ablation Procedure Changed My Patient’s Life
My patient’s voice cracked as she told me she hadn’t slept through the night in three years. She sat across from me in my Huntsville office, tired in a way you can see in someone’s eyes.
Chronic rhinitis had taken her rest. It also took her energy, her patience, and a lot of her hope.
Have you ever felt like you could not get a full breath through your nose, even when you tried everything? Do you feel like your nose just won’t stop draining, no matter what you do?
My patient had that feeling day after day. She felt stuffed up at night. She woke up with a runny nose and a throat that felt raw from postnasal drip. She kept tissues in her car, her purse, and her nightstand.
That first visit mattered to me because it showed a problem that I see all the time. Chronic nasal congestion, nasal drainage, and post-nasal drainage all affect a huge number of people, yet many suffer longer than they should because they do not know there are advanced nasal procedures for chronic rhinitis treatment. One option that often gets missed is the posterior nasal nerve ablation procedure (PNNA).
In this article, I’m going to walk you through my patient’s story, what the procedure is, what the day looks like, what the months after can feel like, and who should consider it.
The patient who changed my perspective on posterior nasal nerve ablation
My patient told me her symptoms started as “just annoying.” Then they slowly became constant. At first, she managed with over-the-counter options. Later, she tried prescription sprays. She tried to power through workdays with a congested and draining nose. At night, she propped herself up on pillows. She still woke up feeling like she could not breathe through her nose or get her nose to stop draining.
That lack of sleep did not stay in the bedroom. It followed her into everything.
Some days she felt foggy at work. She had trouble focusing because her nose and throat kept demanding attention. She felt embarrassed by the constant runny nose and the sniffing. She stopped enjoying simple things, like sitting through a movie without reaching for tissues or waking up feeling calm.
At home, she told me she was “shorter” with her family than she wanted to be. She was exhausted. When your body never gets real rest, your mood pays the price.
What my patient had already tried
My patient had worked hard to fix this. She had tried what many people try first.
Before I talk about a procedure, I want to understand what you have already done, what helped, what did not help, and what you could not tolerate.
She had tried long-term daily routines and still felt stuck. That pattern is familiar in chronic rhinitis treatment. The “Rhinitis 2020” practice parameter update describes how common it is to start with treatments like intranasal corticosteroids, intranasal antihistamines, intranasal anticholinergics, and other medication options, and it also notes that cough can be a symptom in both allergic and nonallergic rhinitis.
My patient’s story also fits what research says about how common nasal symptoms really are. A large survey in the United States found that many people report nasal symptoms over the course of a year, and the estimates shift depending on how rhinitis is defined and whether a doctor diagnosis is involved.
In their survey, almost half of Americans reported troublesome nasal symptoms on at least 7 days in the past 12 months, and the reported prevalence varied depending on the definition used.
How she discovered posterior nasal nerve ablation
My patient told me she finally started searching online late at night. She did what many people do. She typed in questions like: “Why am I always congested?” “”Why is my nose always draining?” Is there a procedure for chronic rhinitis?” “How do you stop postnasal drip?”
That is also common. One study looked at what people search online about posterior nasal nerve ablation and found that many questions focus on basic facts about chronic rhinitis and treatment options. They also found a lot of material online is hard to read and often low quality.
My patient came in asking if there was something beyond “another spray.” That was the opening for a real conversation.
The first visit and assessment
In that first appointment, I focused on two things:
- Understanding her symptoms and pattern: congestion, runny nose, postnasal drip, sneezing, itching, cough, sleep disruption.
- Making sure chronic rhinitis made sense as the working diagnosis: because many problems can mimic each other, and a procedure only helps when we target the right cause.
This is where an ENT surgeon in Huntsville can add value. I can look deeper, ask the questions that matter, and talk through the full set of options.
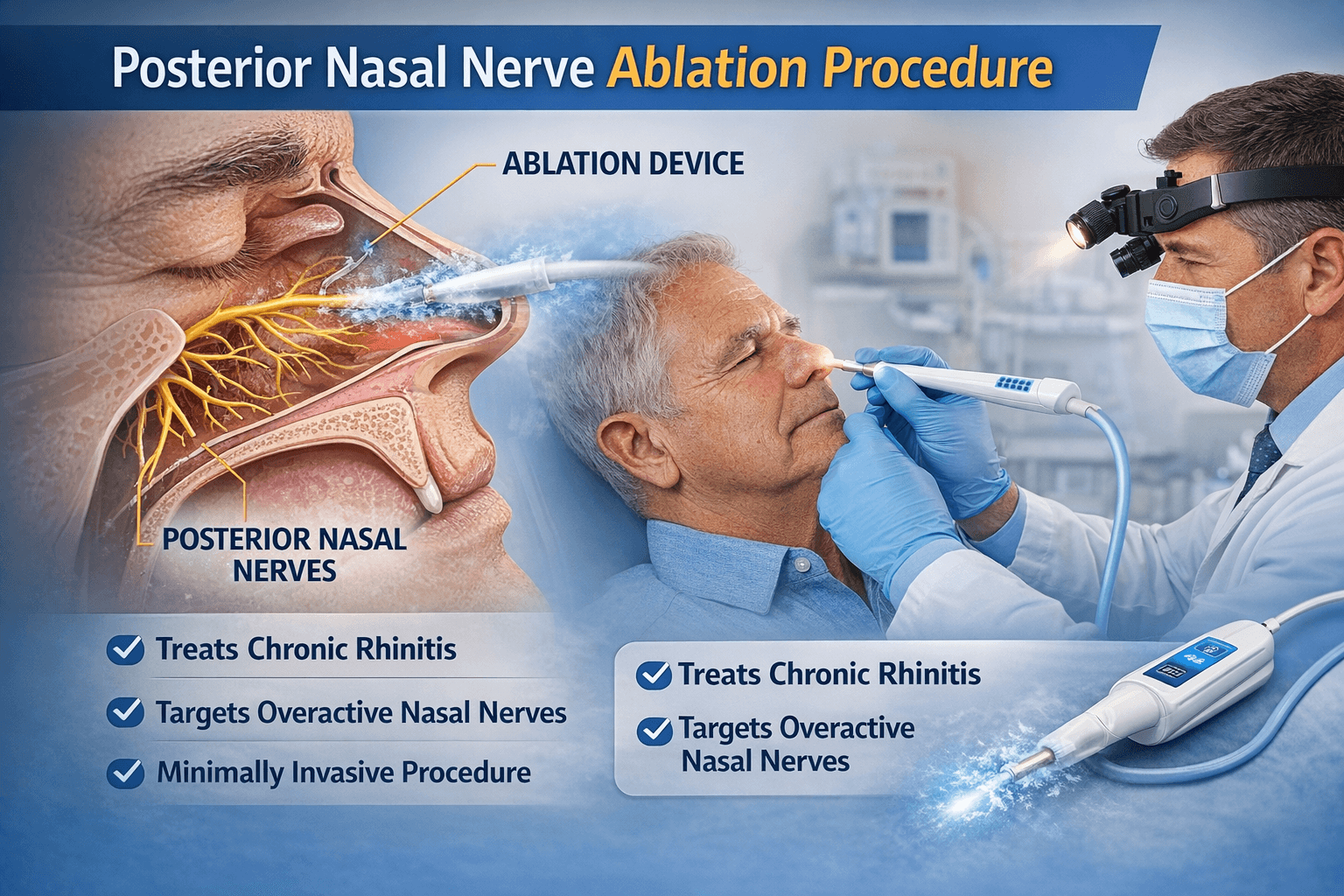
Understanding the nasal nerve ablation procedure
What is “nerve ablation”?
Inside the back part of the nose, there are nerves that help control blood flow and mucus production. In chronic rhinitis, that nerve pathway can act overactive. That overactivity can feed symptoms like a runny nose, congestion, and postnasal drip.
Posterior nasal nerve procedures aim to calm that pathway.
The American Academy of Otolaryngology, Head and Neck Surgery (AAO-HNS) explains that reducing parasympathetic innervation to the nasal cavity can improve symptoms, and that newer interventions focus on the posterior nasal nerves (PNN) because they can be accessed through the middle meatus and are suited for minimally invasive, PNN-targeted procedures. Their position statement supports the use of PNN ablation for medically refractory chronic rhinitis and states these treatments are not considered experimental.
The American Rhinologic Society (ARS) also supports posterior nasal nerve ablation for chronic rhinitis, including allergic and nonallergic subtypes, and states it should not be considered experimental.
So, what does the nasal nerve ablation procedure actually look like in real life?
Two common methods: cryotherapy and radiofrequency
PNN “ablation” can be done using different energy methods:
- Cryotherapy (freezing): A controlled freeze is applied to the target area.
- Radiofrequency neurolysis (low-temperature RF energy): Energy is applied to treat the tissue over the target nerve region.
AAO-HNS notes that multicenter, patient-blinded, sham-controlled randomized controlled trials have shown benefit for both radiofrequency ablation and cryoablation.
I also like patients to know that studies have measured symptom improvement using tools like total nasal symptom scores and quality-of-life surveys.
For example:
Why this can help when medications do not
Medications can help many people, and they remain first-line. The practice parameter update, as mentioned above, describes options like intranasal corticosteroids and intranasal antihistamines, and it highlights how treatment selection can differ for allergic and nonallergic rhinitis.
But even with good care, some people keep struggling.
When symptoms persist despite medical management, procedures that target the posterior nasal nerve can be an option. AAO-HNS describes this approach as a way to address symptoms by targeting distal branches rather than older, more invasive options like vidian neurectomy, which carries risks such as dry eye.
The “minimally invasive” part
When I say “minimally invasive,” I mean:
- It can often be done in-office under local anesthesia.
- It does not require incisions.
- Many people go home the same day.
The procedure can take about 30 minutes and is a same-day treatment.
The day everything changed: May patient’s nasal nerve ablation experience
By the time my patient scheduled her nasal nerve ablation, she was ready. Still, nervousness is normal.
Before we started: preparation and mindset
I reminded her that the procedure targets the posterior nasal nerve region and that we use local anesthesia to reduce discomfort. We discussed what she might feel during treatment, like sensations like pressure, mild discomfort, and the sound of the radiofrequency ablator in action.
I also set expectations for the early days after. Many people have some temporary swelling, congestion, sensitivity, or crusting as healing happens.
Temporary congestion and crusting can occur for just a few weeks while the nasal passage heals.
During the procedure: step by step
Here is how I explain it to my patients:
- Numbing the nose: I apply local anesthesia inside the nose. The goal is comfort.
- Visualizing the target area: I use a thin endoscope so I can see the area I need to treat.
- Treating the posterior nasal nerve region: Depending on the method, I apply controlled freezing or low-temperature radiofrequency energy to the tissue over that nerve-rich region.
- Finishing up and checking in: I make sure bleeding is minimal, review aftercare again, and confirm the patient feels steady before leaving.
Most patients want to know, “Will I feel pain?” In the RhinAer patient FAQ, it states that most patients experience little to no discomfort during treatment because local anesthesia numbs the inside of the nose. I also tell patients there can be discomfort afterward, but it is often manageable.
A systematic review of ClariFix cryotherapy studies reported minor adverse effects such as post-procedural pain or discomfort, headache, and palate numbness, with no major adverse events identified in the included studies.
That does not mean “nothing can happen.” It means we take risks seriously, talk about them clearly, and plan for them.
Right after: her first impressions
My patient sat up and blinked like she was checking if this was real. She told me it felt strange, but not unbearable. She felt pressure more than pain.
Before she left, I gave her simple aftercare steps. As the AAO-HNS Bulletin article described, using saline sprays frequently and avoiding nose blowing for a few days, plus using acetaminophen and ibuprofen for discomfort. That advice aligns with what I recommend. I as well often will recommend saline rinses with antibiotic ointment mixed in for about two weeks after the procedure.
The first night she slept through
This is the part I will not forget.
She sent a message after her first night. She said she slept through without waking up to that stuffed-up panic, and that her nasal drainage had reduced substantially. She did not say every symptom vanished overnight. She said something more powerful: she finally rested.
Six months later: The ripple effects of successful treatment
Six months later, she walked into my office with a different face.
She looked lighter.
She told me her nose felt calmer. She was not constantly bracing for the next wave of congestion. She did not carry tissues everywhere “just in case.” She still paid attention to her body, but it no longer controlled her day.
Better breathing and reduced nasal drainage was only the start
She described changes that surprised her.
She had more patience at home. She did not feel as snappy, because she was not running on empty. She said mornings felt less miserable. Many surveys show mornings can be a hard time for people with allergic rhinitis symptoms.
A survey about patient perceptions and quality of life reported that people with allergies often describe symptoms as disruptive to daily life, with severe symptoms commonly in the morning, and that restoring normal breathing is a top desired effect of treatment.
My patient’s experience matched that theme. Breathing better improved her sleep. Sleep improved her energy. Energy improved how she showed up everywhere else.
Work and relationships
At work, she felt sharper. She said she could stay in conversations without that constant background distraction. She felt more confident because she was not worried about a runny nose in the middle of a meeting.
At home, she felt more present. She laughed more. She planned things again, because she no longer assumed she would feel miserable.
Advocacy and the “why didn’t I know about this?”
My patient also had a new frustration: “Why did nobody tell me this existed earlier?”
I hear that often.
One study found many online resources about posterior nasal nerve ablation are difficult to read. When information is confusing, people delay care. Or they believe the only options are “live with it” or “take sprays forever.”
Long-term durability: what the studies show
My patient wanted to know if results last. One study reported durable improvement in chronic rhinitis symptoms through 52 weeks after temperature-controlled radiofrequency neurolysis. A longer follow-up on temperature-controlled RF ablation showed sustained improvement at 3 years. A large reduction in symptom scores at 3 years and noted no adverse events were reported between 24 and 36 months in that study.
Who should consider Nasal Nerve Ablation
Not every stuffy or runny nose needs a procedure.
Signs you may be a good fit
From my clinical practice, I consider nasal nerve ablation when someone has:
- Chronic rhinitis symptoms that last months and keep coming back
- Nasal congestion and rhinorrhea that do not respond well enough to medical therapy
- A strong desire to reduce daily medication burden
- Symptoms that affect sleep, work, relationships, or day-to-day comfort
- Anatomy and comfort level that make an in-office procedure reasonable
An AAO-HNS Bulletin article on PNN ablation techniques emphasizes the importance of confirming diagnosis, ruling out other causes, and using nasal endoscopy as part of the workup, as well as identifying issues that might make an office procedure a poor fit, such as significant anxiety with procedures or certain anatomic issues that may require different management.
A RhinAer patient FAQ also notes a candidacy idea based on symptom scoring and stresses that the best way to know is a consultation because nasal anatomy and needs differ.
What the consultation process looks like
When you come in to see me, I focus on clarity.
I will ask:
- What are your main symptoms: runny nose, congestion, sneezing, itching, postnasal drip, cough?
- How long has this been going on?
- What have you tried, and what happened with each attempt?
- What bothers you most: sleep, work, voice, exercise, social life?
Then I look, because symptoms alone are not enough.
A careful evaluation and endoscopic exam help rule out other conditions and help decide whether an in-office procedure makes sense. This step also helps us talk honestly about expected outcomes and risks.
Risks and side effects
Commonly discussed side effects include pain or discomfort, headache, crusting, and bleeding. The same study above reported minor adverse effects such as:
- pain or discomfort
- Headache
- palate numbness
No major adverse events were identified in that set of studies.
However, bleeding can be serious in rare cases. A multi-center case series reported severe epistaxis requiring surgical intervention after PNN ablation, stating severe epistaxis occurred in 2% of cases and could occur on average about 20 days after the procedure.
This is why I give clear aftercare instructions and why I want patients to call if something feels wrong.
Final words
My patient’s transformation after her nasal nerve ablation procedure reminded me that chronic rhinitis is not “just allergies” for many people. For some, it is years of poor sleep, daily frustration, and constant nasal symptoms that steal comfort and confidence.
If you are dealing with chronic nasal congestion and runny nose that have not improved with standard treatments, you do not have to keep guessing. Schedule a consultation to discuss whether nasal nerve ablation could be a fit for your symptoms, your goals, and your life.
Frequently Asked Questions
How painful is nasal nerve ablation?
Discomfort is often described as mild to moderate and manageable. The RhinAer patient FAQ states most patients experience little to no discomfort during treatment because local anesthesia numbs the inside of the nose.
What is recovery time like?
Most patients go home the same day. Mild discomfort, swelling, and congestion can occur for a few days and can be managed with simple pain relief and saline douches. The RhinAer patient FAQ notes that many patients return to normal activities with minimal to no downtime, and it mentions temporary congestion and crusting as healing happens.
Sources
- Dykewicz, M. S., Wallace, D. V., Amrol, D. J., Baroody, F. M., Bernstein, J. A., Craig, T. J., Dinakar, C., Ellis, A. K., Finegold, I., Golden, D. B. K., Greenhawt, M. J., Hagan, J. B., Horner, C. C., Khan, D. A., Lang, D. M., Larenas-Linnemann, D. E. S., Lieberman, J. A., Meltzer, E. O., Oppenheimer, J. J., Rank, M. A., Shaker, M. S., Shaw, J. L., Steven, G. C., Stukus, D. R., & Wang, J. (2020). Rhinitis 2020: A practice parameter update. American Academy of Allergy, Asthma & Immunology.
- Nathan, R. A., Meltzer, E. O., Derebery, J., Campbell, U. B., Stang, P. E., Corrao, M. A., Allen, G., & Stanford, R. (2008). The prevalence of nasal symptoms attributed to allergies in the United States: Findings from the burden of rhinitis in an America survey. Allergy and Asthma Proceedings, 29(6), 600–608.
- American Academy of Otolaryngology–Head and Neck Surgery. (2023, January 17). Position statement: PNN ablation for the treatment of chronic rhinitis.
- American Rhinologic Society. (2022, January). ARS position statement: Posterior nasal nerve ablation.
- Del Signore, A. G., Greene, J. B., Russell, J. L., Yen, D. M., O’Malley, E. M., & Schlosser, R. J. (2022). Cryotherapy for treatment of chronic rhinitis: 3-month outcomes of a randomized, sham-controlled trial. International Forum of Allergy & Rhinology, 12(1), 51–61.
- Ehmer, D., McDuffie, C. M., Scurry, W. C., Jr., McIntyre, J. B., Mehendale, N. H., Willis, J. H., Shealy, R. B., Watkins, J. P., & Kakarlapudi, V. V. (2022). Temperature-controlled radiofrequency neurolysis for the treatment of rhinitis. American Journal of Rhinology & Allergy, 36(1), 149–156.
- Aerin Medical Inc. (n.d.). How RhinAer® treats chronic rhinitis: Patient FAQs.
- Desai, V., Sampieri, G., Namavarian, A., & Lee, J. M. (2023). Cryoablation for the treatment of chronic rhinitis: A systematic review. Journal of Otolaryngology – Head & Neck Surgery, 52, 37.
- Canonica, G. W., Mullol, J., Pradalier, A., & Didier, A. (2008). Patient perceptions of allergic rhinitis and quality of life: Findings from a survey conducted in Europe and the United States. World Allergy Organization Journal, 1(9), 138–144.
- Gorelik, D., Razmi, S. E., Sims IV, R. K., Dhanda, A. K., Takashima, M., Brissett, E. S., Rowan, N. R., & Yim, M. T. (2024). Patient questions surrounding posterior nasal nerve ablation for chronic rhinitis. OTO Open. Advance online publication.
- Stolovitzky, J. P., Ow, R. A., Silvers, S. L., Bikhazi, N. B., Johnson, C. D., & Takashima, M. (2021). Effect of radiofrequency neurolysis on the symptoms of chronic rhinitis: A randomized controlled trial. OTO Open, 5(3), 2473974X211041124.
Related Posts
The Wonderful Cakes


